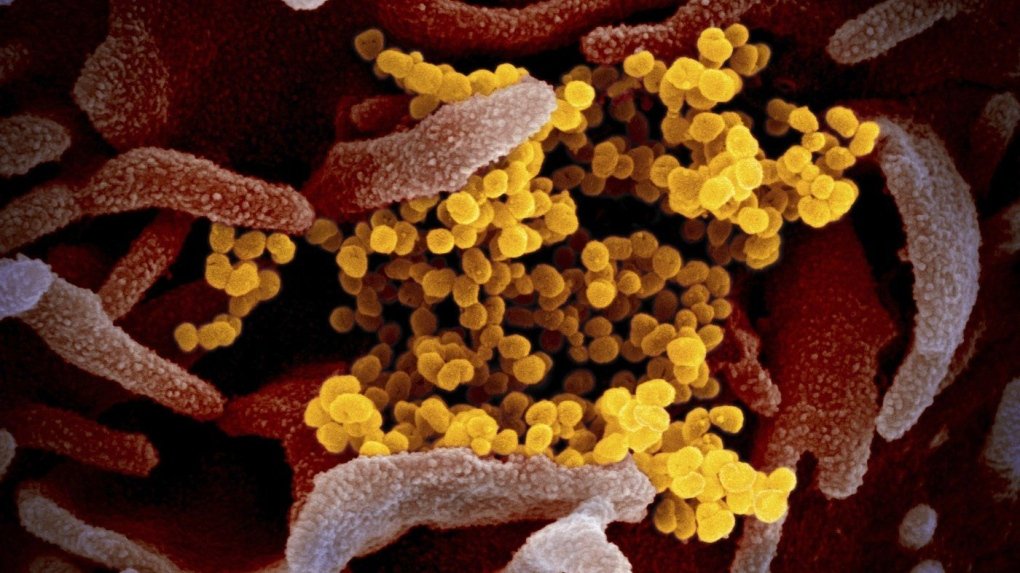
Five years ago, a group of people in Wuhan, China, fell ill with a virus never before seen in the world.
The germ had no name, nor did the disease it would cause. It ended up triggering a pandemic that exposed deep inequalities in the global health system and reshaped public opinion on how to control emerging deadly viruses.
The virus is still with us, although humanity has developed immunity through vaccines and infections. It is less deadly than in the early days of the pandemic and no longer tops the list of leading causes of death. But the virus is evolving, which means scientists need to monitor it closely.
Where did the SARS-CoV-2 virus come from?
We don’t know. Scientists believe the most likely scenario is that it circulated in bats, like many coronaviruses. They believe it then infected another species, probably raccoon dogs, civet cats or bamboo rats, which in turn infected humans who handled or slaughtered those animals at a market in Wuhan, where the first human cases appeared in late November. of 2019.
This is a known route of disease transmission and probably triggered the first epidemic of a similar virus, known as SARS. But this theory has not been proven for the virus that causes COVID-19. Wuhan is home to several research laboratories involved in collecting and studying coronaviruses, fueling debate over whether the virus may have leaked from one of them.
It is a scientific enigma that is difficult to solve under the best of circumstances. The effort has been made even more challenging by political criticism over the origins of the virus and by what international researchers say are measures by China to hide evidence that could help.
The true origin of the pandemic may not be known for many years, if ever.
How many people died from COVID-19?
Probably more than 20 million. The World Health Organization has said member countries have reported more than 7 million deaths from COVID-19, but the true death toll is estimated to be at least three times higher.
In the United States, an average of about 900 people per week died from COVID-19 over the past year, according to the U.S. Centers for Disease Control and Prevention.
The coronavirus continues to affect older adults more. Last winter in the U.S., people 75 and older accounted for about half of the country’s COVID-19 hospitalizations and in-hospital deaths, according to the CDC.
“We cannot talk about COVID in the past as it is still among us,” said WHO director Tedros Adhanom Ghebreyesus.
What vaccines were available?
Scientists and vaccine manufacturers broke speed records in developing COVID-19 vaccines that have saved tens of millions of lives around the world and were the critical step in returning life to normal.
Less than a year after China identified the virus, health authorities in the United States and Britain approved vaccines made by Pfizer and Moderna. Years of previous research, including Nobel-winning discoveries that were key to making the new technology work, gave so-called mRNA vaccines an advantage.
Today, there is also a more traditional vaccine made by Novavax and some countries have tested additional options. The rollout in poorer countries was slow, but the WHO estimates that more than 13 billion doses of COVID-19 vaccines have been administered worldwide since 2021.
Vaccines are not perfect. They do a good job of preventing serious illness, hospitalization, and death, and have been shown to be very safe, with serious side effects infrequent. But protection against milder infections starts to wane after a few months.
Like flu vaccines, COVID-19 vaccines must be updated periodically to adapt to the ever-evolving virus, contributing to public frustration with the need to get vaccinated repeatedly. Efforts are underway to develop next-generation vaccines, such as nasal vaccines that researchers hope can better block infection.
Which variant dominates now?
Genetic changes called mutations occur when viruses make copies of themselves. And this virus has proven to be no different.
Scientists named these variants with Greek letters: alpha, beta, gamma, delta and omicron. Delta, which became dominant in the US in June 2021, raised many concerns because it was twice as likely to cause hospitalization as the first version of the virus.
Then, at the end of November 2021, a new variant appeared: omicron.
“It spread very quickly,” taking over within weeks, said Dr. Wesley Long, a pathologist at Houston Methodist in Texas. “It produced a huge increase in cases compared to anything we’ve seen before.”
But on average, the WHO said, it caused less severe illness than delta. Scientists believe this may be partly because immunity had been developing due to vaccination and infections.
“Since then, we continue to see these different omicron subvariants accumulate more different mutations,” Long said. “Right now, everything seems locked on this omicron branch of the tree.”
The omicron relative now dominant in the U.S. is called XEC, which accounted for 45% of the variants circulating nationally in the two-week period ending Dec. 21, the CDC said. Existing COVID-19 drugs and the latest booster vaccine should be effective against it, Long said, since “it’s actually kind of a remix of variants that are already circulating.”
What do we know about long COVID?
Millions of people remain in limbo with a sometimes disabling and often invisible legacy of the pandemic called long COVID.
It can take several weeks to recover after a COVID-19 attack, but some people develop more persistent problems. Symptoms that last at least three months, sometimes for years, include fatigue, cognitive problems known as “brain fog,” pain, and cardiovascular problems, among others.
Doctors don’t know why only some people get long COVID. It can occur even after a mild case and at any age, although rates have decreased since the early years of the pandemic. Studies show that vaccination can reduce the risk.
It’s also unclear what causes long COVID, complicating the search for treatments. One important clue: More researchers are finding that traces of the coronavirus can persist in some patients’ bodies long after their initial infection, although that can’t explain all cases.
The Associated Press Health and Science Department receives support from the Howard Hughes Medical Institute’s Scientific and Educational Media Group. The AP is solely responsible for all content.